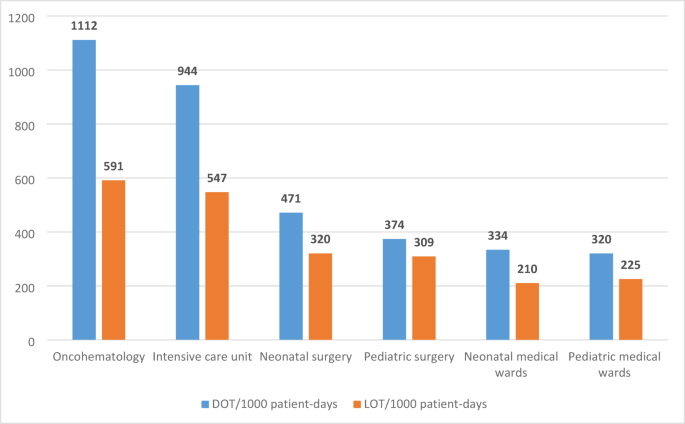
Our analysis of antibiotic consumption administered in an Italian tertiary care academic children hospital in 2022 showed a DOT and LOT/1000 patient-days equal to 539 and 354, respectively; the DOT/LOT ratio was equal to 1.5. Antibiotic consumptions were the highest in oncohematology and ICU wards with a DOT/1000 patient-days of 1,112 and 944 and a LOT/1000 patient-days of 591 and 547, respectively.
A small number of studies used data on antibiotic prescriptions dispensed to hospitalized pediatric patients to estimate their consumption using DOT/1000 patient-days as an indicator. A study conducted in a tertiary care children hospital in London from 2010 to 2018 estimated a median antibiotic consumption of 617 DOT/1000 patient-days in non-ICUs and 1,413 DOT/1000 patient-days in pediatric ICU5. Our results were lower than that reported in the literature; nonpharmaceutical interventions for controlling COVID-19 spread were still in place in 2022 affecting the transmission of many respiratory viruses, and reducing Emergency Department visits and hospitalizations due to acute respiratory infections7 that are frequently treated with unnecessary antibiotics. However, comparisons between institutions are challenging, being influenced by the patient population and the range of interventions undertaken in each setting5.
As we documented in a previous multicenter study6, DOT and LOT/1000 patient-days were higher in males with respect to females. Prevalence of antibiotic use in Italy in 2022 was slightly higher in males than females in all age classes, in particular in the 0–1 year age group (35.7% vs. 32.3%). In terms of consumption, in the age group 2–5 years, there are more marked differences between males and females than in the other age groups, with males exceeding 938 packs per 1000 children compared to 879 packs/1000 in females8,9. Analysis by single antibiotic molecule showed that piperacillin/tazobactam, meropenem and sulfamethoxazole/trimethoprim were the drugs with the highest DOT, although they were not the most prescribed; this could be due to the use of these molecules for long periods either for treatment of severe infections (e.g. meropenem; piperacillin/tazobactam)10 or for medical prophylaxis in immunocompromised children (e.g. sulfamethoxazole/trimethoprim)11. Meropenem had a high DOT (59.6 DOT/1000 patient-days); it is frequently used to treat serious infections, such as bloodstream infections, especially in patients with chronic underlying diseases6. This may be one reason why meropenem resulted to be widely used in oncohematology (176 DOT/1000 patient-days) and in ICU (128 DOT/1000 patient-days). In contrast, cefazolin represented the molecule with the highest number of prescriptions but had a lower DOT of 51.3 DOT/1000 patient-days. Cefazolin is the most commonly used antibiotic for perioperative prophylaxis because of its efficacy, low cost, duration of action, and spectrum of activity12. Surgical prophylaxis represents one of the main indication for antibiotic prescription in hospitalised children6, and the administration of only one preoperative dose is recommended13. This can explain the high number of cefazolin prescriptions observed in our study, and its low DOT. With regard to the use of AWaRe antibiotics according to the WHO classification14, we reported consumptions related to molecules belonging to the “Reserve group”, meaning antibiotics that should be reserved for treatment of confirmed or suspected infections due to multi-drug-resistant organisms (e.g. ceftazidime/avibactam). This result could be due to the higher prevalence of multidrug-resistant microorganisms in Italy compared to other European countries15.
The analysis by type of ward showed that oncohematology had a DOT/1000 patient-days equal to 1,121, higher than other clinical wards; this is in line with what was observed from a study conducted in Italy on antibiotic prescriptions and prophylaxis in Italian children in 201616. Children with oncologic or hematologic diseases are at particularly high risk for severe infections, especially while on chemotherapeutic treatment, radiation, or after stem cell transplantation17,18. Among children treated in pediatric cancer centers, the high prevalence of and risk for adverse outcomes related to severe bacterial and fungal infections lead to a high level of antimicrobial prescribing, for both treatment and prophylaxis18. Our data confirmed that oncologic and hematologic patients were responsible for a large proportion of antibiotic consumption with the highest use of polypharmacy (DOT/LOT ratio 1.9).
With respect to studies that are based on information collected manually from patients’ medical clinical records, we had no need to restrict the sample size. Moreover, the data useful for the study derived from patients’ EMRs which provide the most detailed information of patient clinical and demographical characteristics and of the prescribed treatments. Our study has some limitations. Firstly, it was a monocentric study, therefore results cannot be considered representative of the whole country. The analysis focused on inpatient prescribing alone and did not includes corresponding clinical data regarding the indications for antimicrobial use, or the complexity and acuity of patient population.
In conclusion, our results indicate that the availability of EMRs can greatly improve the accessibility of data to calculate DOT and LOT of antibiotics with the ability to calculate these indicators in an automated and routine manner and use them as part of antibiotic stewardship programs.
link






More Stories
UniHealth Hospitals Limited Announces the Commissioning of its Advanced Tertiary Care, Multi-Specialty Hospital in Navi Mumbai
Predictors of opportunistic infections among people living with HIV: a prospective cohort study from a tertiary care setting in India
The impact of DRG payment reform on inpatient costs for different surgery types: an empirical analysis based on Chinese tertiary hospitals