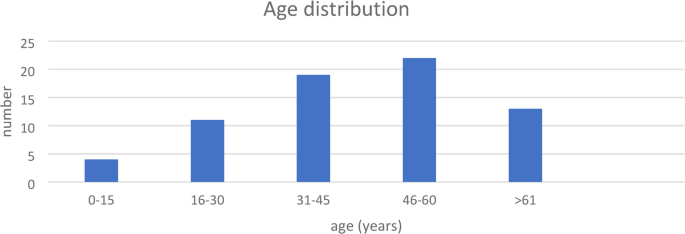
Ruptured liver abscess remains a challenging condition for surgeons because of its high morbidity and mortality rates, especially when associated with systemic illness and comorbidities. In our study, a strong male predominance (88.4%) was observed (Tables 1 and 4) which is consistent with findings by Memon et al. (80.4%)14 and Mohit et al. (86%)15. This may be attributed to increased alcohol consumption, which is socially predominant among males in many regions. The most affected age group was 46–60 years (31.9%) ( Tables 1 and 4 Fig. 1), which aligns with Mohit et al. report (40–50 years)15 and studies by Parihar et al.16 and Alam et al.17 (Table 18), suggesting that the peak incidence occurs in middle-aged to elderly patients due to comorbidities such as diabetes and chronic liver disease (Table 5; Fig. 2) .
The most common symptoms in our cohort were abdominal pain (100%) and fever (76.8%), which is consistent with the findings of similar studies. Memon et al. reported fever in 100% of cases and abdominal pain in 90% of cases1 (Tables 6 and 9). Laboratory findings revealed elevated white blood cell (WBC) counts (mean 20.2 × 10³/dL), alkaline phosphatase levels (mean 323 IU/L), and bilirubin levels (mean 1.9 mg/dL) (Tables 3, 10 and 11). These findings were also consistent with studies by Sarda et al.18 and Greany et al.19, who reported leukocytosis, elevated ALP, and hyperbilirubinemia as common features.
Ultrasonography (USG) is a key diagnostic tool for accurately locating abscesses and their associated complications. Subcapsular abscesses were most common (39.1%), followed by subdiaphragmatic collections (18.8%) (Tables 7 and 12). This finding is comparable to those of studies by Sarda et al.18 and Madhumita et al.20, which also emphasized the utility of USG in diagnosing complications such as subhepatic and subphrenic abscesses.
Management strategies included initial resuscitation, intravenous antibiotics, and either percutaneous catheter drainage (PCD) or surgical drainage on the basis of clinical severity. PCD was performed in 32 patients (46.4%), whereas 24 patients (34.8%) underwent open drainage. Two PCD patients required subsequent surgery because of failure. The overall mortality rate was 21%, with significantly greater mortality (45.8%) in the surgical drainage group than in the PCD group (3.1%), highlighting the severity of illness in patients requiring open surgery (Tables 2, 8 and 16). This finding was in line with that of Huang et al.11, who reported higher mortality rates in open drainage patients.
The APACHE II score plays a pivotal role in guiding management decisions. Patients who underwent surgical drainage had a significantly greater mean APACHE II score (9 ± 4) than did those who underwent PCD (7 ± 3), indicating that the severity of illness is a key determinant (Tables 15 and 17). Studies by Mischinger et al.21 and Hsieh et al.10 similarly emphasized the correlation between high APACHE II scores (> 15) and the need for aggressive surgical intervention. In contrast, patients with lower scores were managed effectively with PCD or antibiotics alone.
Colonic involvement was observed in 41.6% of surgical patients, with complications such as perforation and necrosis (Table 13; Fig. 3). This association, particularly in amoebic liver abscesses, has been extensively reported. Entamoeba histolytica invades the large bowel, creating ulcers that may progress to perforation, particularly in the cecum22. Mohit et al.15 reported colonic involvement in 17 patients, with surgical interventions ranging from cecal resection to ileostomy.
The duration of hospital stay was slightly longer in open drainage patients (6 ± 4.5 days) than in PCD patients (5 ± 3.8 days), but the difference was not statistically significant (p = 0.409) (Table 15). Similar studies by Singh et al.23 and Baijlal et al.24 reported longer stays for PCD (11.3 and 15 days, respectively) (Table 19), but this discrepancy may reflect differences in institutional protocols and patient follow-up strategies.
Postoperative complications were graded via the Clavien‒Dindo classification. The mean length of hospital stay varied across grades but was not significantly different (Table 14), possibly due to the small sample size. Mentula et al. previously highlighted prolonged hospital stays in patients with higher Clavien–Dindo grades, emphasizing the need for tailored postoperative care26.
Our study underscores the evolving role of PCD as a primary modality for managing ruptured liver abscesses. The shift from traditional surgical drainage to less invasive methods has been driven by advancements in imaging and interventional radiology. However, surgical intervention remains crucial for patients with higher APACHE II scores, PCD failure, or complications such as bowel perforation. Studies by Ochsner et al.27 and Tan et al.28 also support this stratified approach (Table 20), demonstrating the importance of individualized management plans.
In conclusion, our findings highlight the importance of early diagnosis, severity assessment via the APACHE II score, and a multidisciplinary approach for managing ruptured liver abscesses. While PCD offers a safe and effective option for most patients, those with severe disease or complications benefit from timely surgical intervention. Future research should focus on refining predictive models and optimizing care protocols to further improve outcomes.
Limitations of the study
-
A.
Our study is an observational study with less number of patients. A multicentric randomized control study with more sample size will be required to have clinical and statistical significance.
-
B.
Our study comprised of only patients undergoing emergency laparotomy. Hence the results reflect the complex interplay of various factors.
link






More Stories
UniHealth Hospitals Limited Announces the Commissioning of its Advanced Tertiary Care, Multi-Specialty Hospital in Navi Mumbai
Predictors of opportunistic infections among people living with HIV: a prospective cohort study from a tertiary care setting in India
The impact of DRG payment reform on inpatient costs for different surgery types: an empirical analysis based on Chinese tertiary hospitals