This pre-post research was conducted on the medical and health sciences students of the four medical and health colleges at the UoS; College of Medicine (CoM), College of Health Sciences (CHS), College of Dental Medicine (CDM), and College of Pharmacy (CoP). Our research primarily aimed to foster the understanding of medical and health sciences, dentistry and pharmacy students at UoS about PS and quality of care in an IPE setting.
Study settings
The CoM of UoS runs a 6-year integrated and system-based MBBS program using a problem-based curriculum. All three phases of the program, basic sciences, pre-clinical and clinical, boast early clinical exposure and the professional development of medical students with a growing emphasis on PS and IPE. However, through the interprofessional education and practice committee of the four medical and health colleges at UoS, headed by Prof. Salman Guraya, the students and faculty have remarkable readiness and interest towards collaborative education and practice. The CoP offers a pharmacy bachelor program and three postgraduate programs: Master in pharmaceutical sciences, pharm. D, and PhD in pharmaceutical sciences. PS is an essential topic and pivotal in the CoP programs. The CDM offers a 5-year program for the Bachelor of Dental Surgery. The curriculum includes four streams: dental health sciences, dental clinical practice, human biology, and community dentistry. PS module is delivered in clinical settings with an emphasis on the assessment of students’ knowledge and clinical application of the subject. Lastly, the CHS has seven undergraduate 4-year programs: nursing, physiotherapy, medical lab sciences, dietetics and nutrition, diagnostic imaging, environmental health, and health services administration. Currently, PS is interwoven into the curriculum, and there is some emphasis on PS in both theory and practice. However, there are no formal IPE and PS courses in the curricula of all four medical and health colleges of UoS.
Study participants
Senior students (last 2 to 3 years of all programs) from CoM, CoP, CDM, and CHS of the UoS participated in this study. Most of these students were engaged in clinical clerkships during the hospital training part of their curriculum. Following the approval by the Research and Ethics Committee (REC-21–12-12), invitations were sent to all eligible students of four colleges using flyers, registration links, QR codes and consent forms via email blurbs. The interested students were required to sign up for the workshop. A participant information leaflet was distributed to the registered students for their pre-workshop knowledge and orientation. The consent form was signed at the start of the workshop and students completed the questionnaire prior to the start of the workshop. The sample size for this study was calculated to be a minimum of 130 participants, based on a sample comparison of means formula, using a power of study of 90%, and an alpha risk of 5%.
Sampling technique
We employed a stratified convenience sampling technique, where students were recruited from the CoM, CoP, CDM, and CHS at the UoS. Each college served as a stratum, ensuring balanced representation across disciplines. This is a non-probability sampling method where participants were selected based on availability, ease of access, or willingness to participate, rather than random selection. While this method ensures representation across key subgroups, it acknowledges the limitations associated with convenience sampling. This approach enhances transparency in participant selection while contributing to the study’s methodological rigor and credibility.
Study questionnaire and clinical cases for breakout rooms
We developed a customized questionnaire tailored to the specific needs and objectives of our study. The development process began with reviewing existing questionnaires and literature on PS and the quality of care to ensure that relevant domains for our IPE-based intervention were captured appropriately [22,23,24,25,26,27]. We focused on selecting the most relevant statements to align with the research aim of evaluating how the workshop influenced students’ perceptions and insights about PS and the quality of care (Supplementary 1).
After identifying key focus areas, we iteratively tested alternative statements and correlated changes between different versions of the questionnaire. To further refine the tool, we averaged multiple items across domains to minimize the potential for bias or flaws in any single statement. This thorough process resulted in the final instrument containing three main domains: Medical Professionalism (MP) with eight statements, Leadership in Healthcare (LH) with six statements, and Precision Medicine (PM) with five statements. The domain of MP promotes PS by emphasizing an empathetic, patient-centered approach and effective communication [23]. LH supports PS through visionary and collaborative leadership strategies that meet both patient and societal needs [26]. Finally, PM contributes to PS by focusing on individualized treatment plans tailored to each patient’s genetic makeup, environmental, and lifestyle factors. Collectively, these three domains contribute to the broader goals of PS by reinforcing principles such as compassionate care, communication, autonomy, leadership, organizational skills, and teamwork [24]. They are designed to shape attitudes and promote collaborative practice and individualized care [27]. The interrelationship between these domains supports PS by enhancing diagnostic and therapeutic effectiveness under strong professional leadership [25]. The face and content validity of the questionnaire was tested and refined through several rounds of expert review and deliberation, ensuring that the final version accurately reflected the study’s focus on enhancing attitudes and perceptions regarding patient safety and quality of care.
Pre-post workshop
The online workshop was conducted through zoom application and all participants allowed the organizers to record the workshop proceedings. The organizational structure of this 2.5 hr workshop is illustrated in Fig. 1.
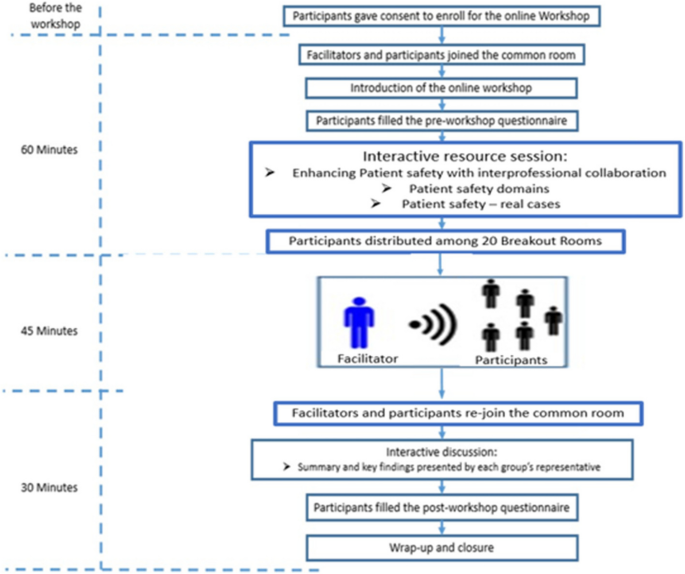
The organizational structure of the pre-post online workshop in the study (n = 248)
After the introduction, and prior to the workshop, all participating students were requested to fill the pre-workshop questionnaire online. The participants were required to answer their responses on a 5-point Likert’s scale from strongly agree, agree, neutral, disagree, and strongly disagree. Subsequently, three interactive resource sessions were delivered about the interchangeable roles of MP, LH, and PM in enhancing the quality of healthcare outcomes by SG, NS, and FJ. Briefly, SG set the scene about the principles and significance of PS and IPE, and NS and FJ discussed the clinical cases, which compromised PS, by using the World Health Organization (WHO) guidelines. During the next phase of the workshop, the participants were distributed into 20 breakout rooms (12–15 students each room with a facilitator) for an inter-professional learning activity in the form of small group discussions. The composition of students in each breakout room ensured, as much as possible, similar representation from each college and discipline, to create a genuine IPE climate. The facilitators represented all four medical and health colleges of UoS, and the workshop demonstrated a genuine case mix of IPE for students and facilitators. The participants were presented four clinical cases with some degree of threats to PS and quality of care. Later, after initial presentations, participants were randomly allocated to breakout rooms where four real practice-based clinical cases were discussed in the form of interactive small group forum. These practice-based real cases were identified by the medical and health sciences students and faculty of UoS during the clinical training. However, it was ensured that all cases were de-identified to maintain confidentiality and to prevent participants from recognizing themselves or others, with strict adherence to ethical guidelines. Broadly, these cases related to medication errors, wrong surgical procedure, and non-compliance with hand hygiene. The domains of IPE and PS in these cases covered medical professionalism, leadership, communication, teamwork, shared decision making, and personalized medicine.
During the breakout rooms, the students were invited to; 1) describe the incident related to PS (e.g., what went wrong?; 2) identify the potential underlying causes; 3) recognize PS and quality of care domains related to the case; 4) analyze the potential measures to prevent the incident; and 5) reflect on how IPE-based practice would contribute to PS in each case. Students were encouraged to interact, brainstorm, and reflect on their opinions under the guidance and assistance of group facilitators. After the small group discussions in the breakout rooms, all students reconvened to the main workshop room, and spokespersons from each breakout room presented a summary of small group discussions and plausible solutions of the discussed clinical scenarios. Finally, all students were requested to fill in the same questionnaire for a pre-post workshop analysis. The workshop was then closed by wrapping up the event and thanking all organizers, students, facilitators, and IT support staff. Prior to the workshop, a dry run was done for the online training of facilitators and organizers for the internet security, breakout rooms dynamics, PowerPoint presentations and equipment check.
Statistical analysis
Data were presented as frequencies with percentages for categorical variables and as median with interquartile (IQR) for ordinal variables. A series of Wilcoxon signed-rank test and McNemar test were conducted to determine if MP, LH, and PM scores and percentages were different at two-point times (pre and post workshop) and if there were significant differences according to the year of study and the college. Moreover, the chi square test was performed to compare the percentages of agreement pre and post workshop. Statistical significance was set at p value ≤ 0.05 (two-sided). The data analysis was performed using the IBM Statistical Package for Social Sciences (SPSS) Statistics for Windows Version 28.0.
link







More Stories
OhioHealth Physician Group Primary Care Earns American Heart Association Awards
Aspirus Stevens Point Hospital Receives 2026 WHA Quality and Patient Safety Award | Press Room
SGMC Health Wins Two Statewide Patient Safety Awards from the Georgia Hospital Association