The characteristics of the neonates
During the study period 19 171 neonates were admitted to the Department of Neonatology and Neonatal Intensive Care and 99 of them died, giving an in-hospital mortality rate of 5.16 per 1000 live births. Its value in the following years was: 2015–8.79, 2016–4.07, 2017–6.32, 2018–4.77, 2019–3.94, 2020–2.34, 2021–8.15, 2022–2.90, 2023–5.79 per 1000 live births.
Both deceased children (N = 99, 0.52%) and children alive at discharge (N = 19 072, 99.48%) were characterized. Socio-demographic variables, maternal related factors and neonatal related factors were analyzed and presented in the Table 1.
In the study group the following variables did not differ between the boys and the girls: gestational age (p = 0.87), birth weight (p = 0.55), body length (p = 0.62), 1-min Apgar score (p = 0.80) and 5-min Apgar score (p = 0.21) (Mann-Whitney U Test). Contrary, in the reference group the boys had significantly higher birth weight and body length than girls (median (Q1-Q3): 3450 (3040–3800) vs. 3300 (2930–3640) g and 56 (53–58) vs. 55 (53–57) cm, respectively) (p < 0.001 in each case, Mann-Whitney U Test).
No differences were found between groups in the following variables: mode of delivery (p = 0.99), maternal age (p = 0.69), gravidity (p = 0.70) and parity (p = 0.64) (Chi-squared test). Compared to the control group, the study group was characterized by a significantly higher proportion of boys (p = 0.01), multiple pregnancies (p < 0.001), outborn neonates (p < 0.001), preterm children (p < 0.001), low birth weight neonates (p < 0.001), children with 1-min Apgar score 0–3 (p < 0.001) and 5-min Apgar score < 7 (p < 0.001) (Chi-squared test). Median birth weight, gestational age, body length, 1-min and 5-min Apgar score of the deceased children were significantly lower than in the alive children (p > 0.001 in each case, Mann-Whitney U Test).
In the next stage of our analysis, the neonates were divided into 4 groups according to their main diagnosis: group E: extremely immature neonates and neonates with extremely low birth weight, group P: premature neonates aged ≥ 28 weeks of gestation and with body weight ≥ 1500 g, group T: term neonates not burdened with genetic disorders, group C: neonates with a severe congenital malformation, deformation, chromosomal abnormality.
The groups were analyzed separately and the results were presented in the Table 2.
Analysis of the clinical problems
In the Group E, 23.44% of the neonates needed resuscitation with epinephrine use in delivery room (N = 15), 4 of them were born with no signs of life. 25.00% of the children (N = 16) had a congenital sepsis/infection and 18.76% (N = 12) had a hospital acquired infection/sepsis. Antenatal corticosteroids were given in nearly 75% of cases requiring this action (N = 44, 74.58%). However, only 54.55% of children were administered a full course of therapy (N = 24).
In the group P, 37.50% of the neonates needed resuscitation with epinephrine use in delivery room (N = 3), 2 of them were born with no signs of life. 25.00% of children (N = 2) had a congenital sepsis. In 87.50% of cases that required it (N = 7), antenatal corticosteroids were not given. In the remaining part, only one dose was administered (N = 1, 12.50%).
In the group C, there were 13 neonates (59.09%) with a lethal congenital malformation/deformation (including: brain defects, kidney defects, thanatophoric short stature and conjoined twins), 5 neonates (22.73%) with a lethal chromosomal abnormality (Edwards’ syndrome, Patau’s syndrome) and 4 (18.18%) children with a malformation syndrome.
The neonates from the group T were briefly characterized.
Patient 1: A neonate admitted from another hospital, undergoing hypothermia therapy, and then receiving palliative care (underlying cause of death – severe birth asphyxia (P21.0); day of death – 36).
Patient 2: A neonate admitted from another hospital in agonal state, died within 24 h of admission (underlying cause of death – neonatal aspiration of meconium (P24.0); day of death – 1).
Patient 3: A neonate treated with nitric oxide, mutation of the EDN1 (Endothelin 1) gene (underlying cause of death – persistent fetal circulation; day of death – 5).
Patient 4: A neonate with trisomy 21, due to intestinal perinatal perforation peritoneal drainage was introduced (underlying cause of death – perinatal intestinal perforation; day of death – 4).
Patient 5: A neonate of a mother without rectal group B streptococcus (GBS) colonization assessment and without perinatal antibiotic prophylaxis (underlying cause of death – sepsis due to Streptococcus, group B; day of death – 7).
Factors associated with the in-hospital mortality of neonates with severe congenital anomalies
The medical records of the children from the group C were analyzed in search for risk factors associated with congenital anomalies in children. In case of 86.36% of the children (N = 19) the mother’s age was < 35 years. All fathers were < 45 years old. No type of mother’s or father’s occupation dominated. 86.36% of the neonates (N = 19) were born from singleton pregnancies. The mothers of 63.64% of the children (N = 19) were multigravida and multiparous. In 13.64% of the cases (N = 3), maternal diabetes was recorded, and in 13.64% (N = 3) – pregnancy-induced hypertension. None of the mothers were diagnosed with pregestational diabetes mellitus or pre-eclampsia. Regarding the history of abortions (spontaneous and induced) and deaths of previous children, they occurred in the case of 5 (22.73%) and 1 (4.55%) children, respectively. All mothers denied the occurrence of the following problems during pregnancy: fever, infectious contact, maternal smoking active or passive, drinking alcohol, taking drugs (medicines), contact with pollutants. We did not find any data regarding periconceptional folic acid, consanguinity and maternal BMI before pregnancy in the patient’s medical records.
Factors associated with the in-hospital mortality of extremely preterm neonates
Univariate and multivariate logistic regression was used to identify which factors are associated with in-hospital mortality of extremely preterm neonates. In the final model of multivariable logistic regression analysis the following predictor variables were associated with the mortality of extremely preterm neonates: gestational age, parity, birth weight percentile, 1-min and 5-min Apgar scores. The detailed data were presented in the Table 3.
Mortality rate and death time analysis
During the study period 99 neonates died (0.52%). There were: 77 early neonatal deaths (77.78%) (of which 42 (54.55%) occurred within the first day of life), 18 late neonatal deaths (18.18%) and 4 postneonatal deaths (4.04%). In the group of children who died in the first 24 h of life 6 deaths occurred under 1 h of life (13.95%), 26 deaths occurred between 1 and 11 h of life (60.47%) and 11 deaths occurred between 12 and 23 h of life (25.58%). The in-hospital mortality rate of preterm neonates was 3.55% (83/2337) and was about 37 times higher than the mortality rate of term neonates (0.10%, 16/16834).
The mortality rates depending on the day of death were: neonatal mortality rate = 4.96 (early neonatal morality rate = 3.81, late neonatal mortality rate = 1.15) and postneonatal mortality rate = 0.21 per 1000 live births.
The mortality rates depending on the gestational age were: 22–23 weeks of gestation = 642.86, 24–25 weeks = 466.6, 26–27 weeks = 197.18, 28–31 weeks = 61.59, 32–36 weeks = 3.68, 37–41 weeks = 0.95 per 1000 live births.
In the group E, 95.31% (N = 61) of all deaths occurred within the first 28 days of life, of which 73.77% (N = 45) occurred within 7 days after birth and 39.34% (N = 24) within 1 day after birth (very early neonatal death). The majority of very early neonatal deaths occurred between 1 and 11 h (N = 18, 75.00%). All deaths from the Group P (N = 8) occurred within the first 28 days of life, of which 75.00% (N = 6) occurred within 7 days after birth and 37.50% (N = 3) within 1 day after birth. 80.00% (N = 4) of neonates from the group T died within the first 28 days of life. All neonates from the Group C died within 7 days after birth (N = 22), of which 68.18% (N = 15) died within the first day of life.
The mortality rate of EPT neonates was 38.36% (61/159). 96.72% (N = 59) of all deaths occurred within the first 28 days of life, of which 71.19% (N = 42) occurred within 7 days after birth and 38.98 (N = 23) within 1 day after birth. In the EPT group, the mortality rates for subsequent weeks of gestation were as follows: 22 weeks – 75.00%, 23 weeks – 60.00%, 24 weeks – 58.06%, 25 weeks – 34.48%, 26 weeks – 25.81%, 27 weeks – 15.00%. Additionally, the mortality rates calculated for VPT and MPT + LPT neonates were: 6.14% (17/277) and 0.32% (5/1901), respectively.
The in-hospital mortality rate of LBW neonates (< 2 500 g) was 4.36% (85/1950) and was about 54 times higher than the mortality rate of neonates with body weight ≥ 2,500 g (0.08%, 12/15191). The mortality rate of ELBW neonates was 33.53% (58/173). 94.83% (N = 55) of all deaths occurred within the first 28 days of life, of which 74.55% (N = 41) occurred within 7 days after birth and 40.00% (N = 22) within 1 day after birth. Additionally, the mortality rates were calculated for VLBW and LBW neonates and were: 6.11% (14/229) and 0.84% (13/1535), respectively.
Survival analysis
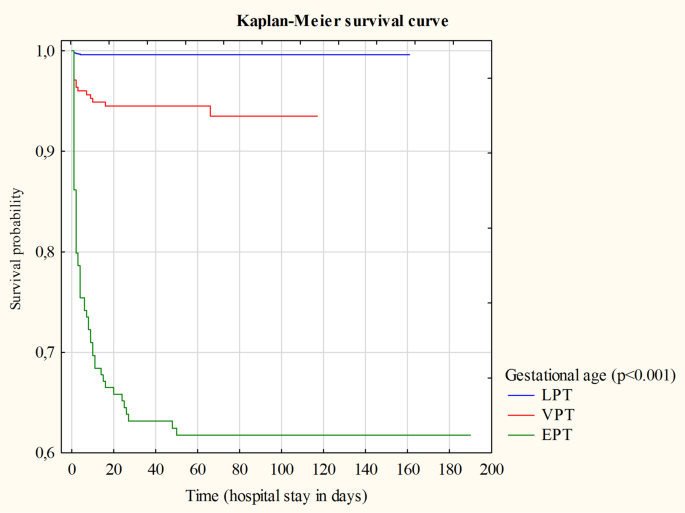
For the preterm neonates admitted to the Department, we generated a Kaplan-Meier survival curves to determine their probability of surviving (Fig. 1). Log-rank test was used to compare survival curves for neonates with different characteristics.

Kaplan-Meier survival curve for preterm neonates – gestational age. LPT – late preterm; VPT – very preterm; EPT – extremely preterm; p – group comparison (log-rank test)
In case of the following factors: week of gestation, birth weight, 1-min and 5-min Apgar scores, significant differences in survival probability were observed (p < 0.001 in each case, log rank survival estimate). Significantly lower survival probability was observed in younger children with lower birth weight and lower 1- and 5-min Apgar scores. Maternal age (p = 0.45), gravidity (p = 0.89), parity (p = 0.74), sex (p = 0.77), birth weight percentile (p = 0.42) and place of residence (p = 0.85) had no effect on the probability of survival (log rank survival estimate).
We generated the Kaplan-Meyer curves for groups separated from the EPT neonates according to the gestational age, body weight, 1-min Apgar score and 5-min Apgar score (Figs. 2 and 3).

Kaplan-Meier survival curve for extremely preterm neonates – 1- and 5-min Apgar scores. p – group comparison (log-rank test).

Kaplan-Meier survival curve for extremely preterm neonates – gestational age and birth weight. p – group comparison (log-rank test)
The underlying causes of deaths
The underlying causes of neonatal deaths fell into two main categories: certain conditions originating in the perinatal period (P00-P96) (N = 77, 77.78%) and congenital malformations, deformations and chromosomal abnormalities (Q00-Q99) (N = 22, 22.22%). The following causes of death were found in the studied groups of children:
Group E: disorders related to length of gestation and fetal growth (N = 61, 95.31%), respiratory and cardiovascular disorders specific to the perinatal period (N = 2, 3.12%) and infections specific to the perinatal period (N = 1, 1.56%);
Group P: respiratory and cardiovascular disorders specific to the perinatal period infections specific to the perinatal period (N = 2, 25.00%), infections specific to the perinatal period (N = 2, 25.00%), conditions involving the integument and temperature regulation of newborn (N = 2, 25.00%), hemorrhagic and hematological disorders of newborn (N = 1, 12.50%) and congenital malformations of the circulatory system (N = 1, 12.50%);
Group T: respiratory and cardiovascular disorders specific to the perinatal period (N = 3, 60.00%), infections specific to the perinatal period (N = 1, 20.00%) and digestive system disorders of newborn (N = 1, 20.00%).
Group C: congenital malformations of the urinary system (N = 7, 31.81%), congenital malformations and deformations of the musculoskeletal system (N = 5, 22.73%), chromosomal abnormalities (N = 5, 22.73%), congenital malformations of the nervous system (N = 2, 9.09%) and other congenital malformations (N = 3, 13.64%).
link






More Stories
UniHealth Hospitals Limited Announces the Commissioning of its Advanced Tertiary Care, Multi-Specialty Hospital in Navi Mumbai
Predictors of opportunistic infections among people living with HIV: a prospective cohort study from a tertiary care setting in India
The impact of DRG payment reform on inpatient costs for different surgery types: an empirical analysis based on Chinese tertiary hospitals