This study analyzed changes in the structure and trends of inpatient costs before and after the implementation of DRG payment reform policies at a tertiary general hospital in Wuhan. The findings revealed that DRG payment reform significantly influenced inpatient cost the structures and dynamics.
The DRG payment policy has a significant effect on controlling hospitalization costs for patients, with a notable reduction in hospitalization expenses. However, the proportion of out-of-pocket expenses have increased. Research has shown that the implementation of the DRG payment policy has led to a significant downward trend in the total hospitalization expenses, which suggested that the DRG payment reform can effectively curb the growth of medical expenses, aligning with previous studies21,22. By establishing payment standards for each disease group, DRG restructures hospitals’ economic incentive mechanisms, driving them to shift from the traditional “fee-for-service” model to a “diagnosis-based payment” system. Hospitals achieved cost reductions by optimizing clinical management pathways, prioritizing cost-effective medication lists, standardizing medical supply protocols, and implementing transparent healthcare quality measures alongside target-based management systems. These measures encouraged medical staff to adopt cost-conscious practices, standardize clinical procedures and select cost-appropriate treatment regimens, thereby reducing patients’ financial burdens23. Additionally, the results found a 16.67% reduction in hospitalization days post DRG payment reform, consistent with Tan et al.24. Length of stay, a key determinant of hospitalization costs, positively correlates with medical expenditures25. As one of the key indicators of DRG, the time consumption index has improved the efficiency and cost awareness of medical staff to a certain extent. By actively carrying out daytime chemotherapy and daytime surgery26,27, medical institutions optimize the diagnosis and treatment process, improve medical efficiency, shorten the hospitalization time of patients, thereby reducing the number of invalid hospitalization days, which effectively reduces the hospitalization expenses of patients.
Despite a decrease in median out-of-pocket expenses for patients after the DRG payment reform, their proportion of total hospitalization costs increased, consistent with Jian et al.28. The increase in the proportion of out-of-pocket expenses has both common causes and differences among different groups (Supplementary Tables S1-2). Specifically, the proportion of elderly patients at their own expense was significantly higher. As the patient’s age increases, the physiological functions decline continuously, and the diseases are characterized by comorbidity and chronicity. It not only increases the complexity and difficulty of treatment, directly leading to the prolongation of hospital stay, but also requires additional expenses for rehabilitation and care. DRG payment may not cover extended costs such as long-term medication and rehabilitation treatment29. Higher surgery complexity also increased costs due to advanced technologies, high-value consumables (e.g., imported equipment, special implants), postoperative special medication, as well as the development and application of new technology and new business30. Occupational groups with different types of medical insurance (e.g., employee medical insurance vs resident medical insurance) face varying reimbursement rates, self-paid upper limit, and disposable income, influencing their willingness to pay for premium treatment and services31, while patients with resident medical insurance are the opposite32. This increase in out-of-pocket expenses partially offset the DRG payment policy in alleviating the problem of “expensive medical treatment”, highlighting the need to consider individual characteristics of patients and diseases in future policy adjustments.
Therefore, dynamically adjusting the DRG disease group catalog, improving the quantity and standards of DRG subgroups, and updating the medical insurance payment catalog by incorporating factors such as surgical complexity level, patient age, and treatment modalities as grouping nodes are necessary to make DRG grouping more scientific and reasonable33. At the same time, a multi-level security system should be built to expand medical insurance coverage, and commercial insurance institutions should be encouraged to develop medical insurance products for elderly patients, such as long-term care insurance, to provide more security options34. These measures can reduce both total and out-of-pocket expenses, effectively addressing “high medical costs”.
DRG payment contributes to a more rational cost structure, but further optimization is needed. The study explored changes in the structure of hospitalization expenses before and after the implementation of the DRG payment policy, and the degree of change was 4.37%, indicating an effect on the structure of hospitalization expenses. The structure of drug costs and health materials costs showed a negative change, with the proportions declining, indicating that reductions in those costs were crucial in lowering overall hospitalization costs. This effectively alleviating the situation of “supporting with drugs” and “supporting medicine by consumption” within the healthcare system and making the structural changes in patients’ hospitalization costs reasonable, which was consistent with previous research4,5. On one hand, since the implementation of the DRG payment policy, hospitals have transformed the ‘status’ of drugs and consumables into operating costs, thus strengthening the management of drug procurement and usage to reduce overall medical costs by optimizing the drug list and limiting the use of high-cost drugs5. On the other hand, the national government has strengthened the management of high-value medical consumables and forced hospitals to strengthen the fine management of high-value medical consumables by using the DRG payment policy. By adjusting the performance distribution and implementing unified coding management for high-value consumables, measures such as information traceability control consumable costs growth35. Moreover, because medical insurance policy controls costs, it has changed clinical use from expensive imported consumables to cost-effective domestic consumables, ensuring the quality of medical care, thereby reducing material waste and reducing the economic burden on patients.
However, this study found that the contribution rate of structural change (CRSV) of drug costs and health material costs were 27.92% and 22.2% respectively, totaling 50.12%, remaining the main factor affecting hospitalization expenses, which was consistent with Ma et al36. Possible reasons include changes in the disease spectrum and new technologies and services development, increasing demand for special drugs and materials. Meanwhile, medical technologies upgrades, increased consumables use during treatment, and growing patients’ health awareness have inclined both patients and doctors to choose expensive drugs or consumables. At the same time, with the competition in the medical industry, unreasonable medical diagnosis and treatment behaviors have also, to a certain extent, have further increased the financial burden on patients23. Therefore, the government should strengthen the supervision and control of the price of drugs and consumables, encourage the normalization of new technologies, and give certain medical insurance policy support. Hospitals should strengthen the supervision and management of drug use and high-value consumables, establish a warning system for abnormal usage, and link usage outcomes to performance evaluations, so as to realize the monitoring of the use of drugs and high-value medical consumables by medical staff.
Medical service costs exhibited the highest correlation with hospitalization expenses (average correlation coefficient: 0.984), with the CRSV of 22.65%, ranking second, and a strong positive pulling on total cost (0.78%), indicating that DRG payment reform encouraged hospitals to prioritize diagnosis and treatment services reflecting technical labor value of medical staff, aligning with the reform expectation of “changing cages for birds”, which was consistent with the research of Zhang et al37. With the development of medical technology, hospitals may introduce more medical service projects, often requiring higher technical standards and more complex procedures. These advanced technologies require higher costs, increasing related medical services. As medical services, a “mixed commodity” with “medical” and “nonmedical” services priced jointly, the labor value of healthcare workers has not yet been fully reflected38. A relevant study39 indicated that medical service item prices in public hospitals in China were relatively low. Appropriately adjusting these prices enhances healthcare institutions’ revenue structures and effectively controls the proportion of unnecessary examinations, tests, and drug expenses. The “Opinions of the General Office of the State Council on Promoting the High-quality Development of Public Hospitals” ([2021] No.18) proposed in 2021 to support public hospitals in optimizing income structures and increasing the proportion of medical service income (excluding drugs, consumables, inspection and laboratory income) in medical income. Therefore, medical insurance institutions should utilize price adjustment as a macro-control tool to advance medical service prices reform. Hospitals should mobilize medical staff enthusiasm, optimize income structure, increase the proportion of medical service income, and reduce expenditures on drugs and consumables40.
In addition, this study also found that the VSV of examination costs and laboratory costs were 0.68% and 0.51% respectively, but their annual average change rates were relatively high, at 7.04% and 4.86% respectively, indicating that in the initial stage of DRG payment implementation, examination costs and laboratory costs showed a phenomenon of “high growth, moderate contribution”, which was also one of the main reasons for the current high medical costs37. On one hand, cost large-scale medical and inspection equipment indirectly increased hospitalization expenses. On the other hand, enhanced medical literacy may lead patients to pursue comprehensive and systematic examinations. Therefore, in the early stage of reform, fine management and control are necessary to prevent these costs from becoming a structural issue. Hospitals should refine clinical pathways through standardized diagnostic panels to eliminate non-indicated testing, while embedding robust cost surveillance mechanisms—particularly targeting high-value or anomalous diagnostic expenditures. Concurrently, incentive structures must incorporate evidence-based testing compliance rates into performance metrics to optimize diagnostic decision-making and rationalize clinical behaviors40. At the same time, efforts should improve medical services homogenization, strengthen information systems interoperability, and promote sharing and mutual recognition of inspection and test results among tertiary hospitals. This will not only improve the utilization efficiency of medical resources and optimize the expense structure, but also further reduce the medical burden on patients.
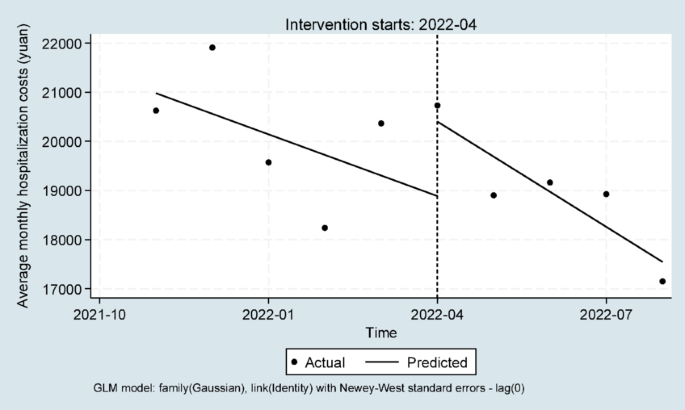
DRG reform exhibits short-term transitional fluctuations, and then a long-term dynamic adjustment mechanism needs to be established. The impact of DRG payment reform on medical expenses and structure presented stage characteristics, with cost control effects varying over time, highlighting differences between short-term and long-term impact41. Although there was a short jump in the total cost, medical insurance expenses, out-of-pocket expenses, drug cost and health material cost at the moment of the implementation of the reform—reflecting adaptive adjustments during policy transition, it decreased significantly over the long term, confirming the inhibitory effect of DRG payment on resource-consuming costs and the continuous effectiveness of cost control4. Notably, the insurance reimbursement share continued to diminish while the out-of-pocket proportion raised commensurately—signaling potential cost-shifting risks that warrant vigilance. For medical service expenses, there was an instantaneous increase in reform but a long-term downward trend. This contrast may be due to the lag of DRG payment dynamic adjustment or the hospital’s reduction of service input under the pressure of cost control. This typical pattern of “short-term fluctuations followed by long-term declines” profoundly reveals the deep-seated effects of the DRG pre-payment system on hospital cost behaviors. Therefore, during the implementation of the DRG payment reform, first of all, we should comprehensively consider various factors and construct a dynamic adjustment mechanism for DRG grouping and payment standards. Establish a regular evaluation system to periodically assess the rationality of DRG grouping. According to the evaluation results, the DRG grouping was dynamically adjusted, and the new diseases, complications and complications were included in the grouping consideration, so that the grouping was more suitable for clinical practice. At the same time, the technical difficulty (CMI), risk degree, resource consumption intensity, medical quality, efficiency and other performance evaluation results of medical services were used as important adjustment factors to reasonably adjust the price of medical services reflecting technical services, so as to avoid hospitals being forced to cut essential services due to insufficient labor value36. Medical institutions should be encouraged to optimize service processes, improve service efficiency, and increase investment in necessary medical services while controlling costs, such as strengthening chronic disease management and health education, so as to enhance the overall level of medical services. Secondly, an intelligent supervision and feedback system should be established. Combined with the management standards of clinical pathways, this system should focus on cost structures and medical quality. Utilize information systems to strengthen key monitoring of diagnosis and treatment behaviors for diseases with rapidly increasing costs. It was necessary to enhance the prevention, control, and supervision of cost-shifting risks. When the proportion of out-of-pocket expenses of medical institutions exceeds a certain threshold, early warning and special verification (especially high-value consumables, special services, off-formulary drugs, etc.) were initiated to prevent hospitals from passing on expenses to patients by increasing out-of-pocket expenses40. Meanwhile, the medical insurance intelligent auditing system should be improved to conduct real-time monitoring of medical cost composition, focusing on abnormal fluctuations in expenses such as medication costs and medical supply costs, and promptly detecting and punishing illegal charges, cost shifting and other behaviors. Finally, incentive mechanisms should be enhanced to promote effective management and enhance resource utilization efficiency in hospitals by establishing and improving cost accounting systems to strengthen internal cost control. In conclusion, by establishing and continuously optimizing a dynamic adjustment mechanism characterized by scientific grouping and pricing, intelligent and precise supervision, and an incentive-compatible orientation, we can effectively cope with short-term fluctuations in hospitalization expenses, prevent structural risks, consolidate the long-term effectiveness of cost control, and ultimately guide the medical system to shift from scale expansion to an intensive development path centered on quality and value.
link






More Stories
Without subsidies, Florida families cringe over health insurance bills
Medicare Advantage Insurers Face New Curbs on Overcharges in Trump Plan That Reins in Payments
Doctors question 6-minute X-ray rule for health insurance payment