Participant demographics and placement information
Eleven eligible participants were identified, of which ten were invited and agreed to participate. The remaining eligible participant left the health service shortly after placement completion and was therefore unavailable. The length of time participants had worked as clinicians ranged from one year and one month to three years and five months, with an average of two years and two months.
The majority of participants (n = 8) were first-time clinical educators, with the remainder (n = 2) being second-time clinical educators. The placements took place in various adult caseloads including acute, rehabilitation, and mental health services, in both hospital and community settings. Some of the participants (n = 4) shared the educator role with a more experienced clinician and all participants only educated one student per placement. The placements ranged in length from five to ten weeks, with the majority being full-time. Of the twelve student placements the participants supervised, ten students passed and two failed the placement.
Educator’s perceptions
There were five main themes identified in the data as summarised in Fig. 1 together with subthemes. Initially, participants had mixed feelings about taking on the educator role (theme 1). They went on to describe how they learned through performing the role. This included adjusting to the responsibilities of the role, resolving challenges (theme 2), and developing the educator and student relationship (theme 3). Participants identified support factors they considered important (theme 4). Overall, through the experience of being an educator, participants reported improved educator, clinical, and professional skills and confidence (theme 5).
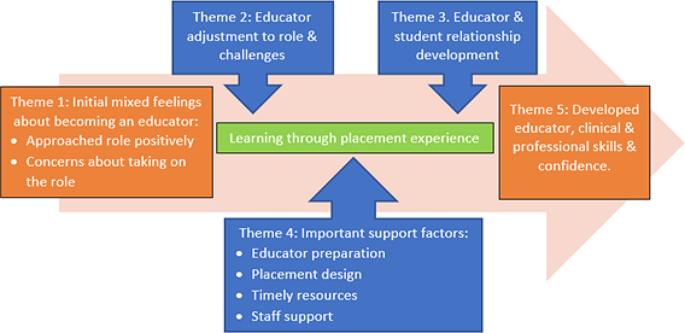
Early career clinical educator experiences and support needs
Theme 1: Initial mixed feelings about becoming an educator
The mixed feelings expressed by participants were categorised into subthemes of how they of approached the role positively and their concerns about taking on the educator role.
Approached role positively
All the participants felt positive about taking on the educator role. Many of the participants stated they felt “excited” and viewed being an educator as “a valuable learning opportunity” (P9). Participants also appreciated the importance of providing placement learning opportunities to support students’ skill development. The notion that taking on the clinical educator role supported participants’ career progression was also expressed: “I was excited to have a student to go the next step in my job as an OT [occupational therapist]” (P6).
Concerns about taking on the educator role
Participants voiced concerns about balancing the educator role with their other clinical duties: “I was nervous about how I was going to juggle my clinical tasks and the student” (P10). The type of student they might be allocated also caused some “hesitation or anxiety” (P7). Many participants voiced feeling “overwhelmed” by the numerous placement resources available to assist them in the educator role. A common experience was participants feeling that they were still learning themselves. They described a lack of clinical and educator experience and confidence, with one participant admitting that she “wasn’t confident really at all…. cause you just don’t know what to expect” (P1). Another participant, referring to her student, questioned, ‘Do I know enough to give you a good placement experience? and am I going to be able to answer all your questions? …” (P2).
Theme 2: Educator adjustment to the role and challenges
Participants spoke of several aspects of the educator role that required them to adjust to a new way of working that they had not anticipated. One aspect was the need to frequently explain what they were doing and why: “It’s just weird, having someone there all the time, making sure that I verbalise everything that I’m thinking about when we’re seeing a patient” (P5). Additionally, the need to be continuously cognisant of where their student was and what activity their student was engaged in took some adjustment: “I constantly felt that responsibility to make sure that they had stuff to do, or that I was telling them what I was doing so they were a bit aware and that whole aspect of it I found more draining than I thought, but I’d do it again easily, but I guess I just didn’t anticipate it” (P2 ).
Many participants described how managing the “competing demands” (P10) of fulfilling clinical, non-clinical, and educator duties to be challenging at times. Simultaneously training and supporting new staff, caseload pressures due to staff absence, or students not performing as expected were added difficulties reported by some participants. The experience that it “can be challenging just not having that space to yourself sometimes” (P9) was shared by several participants. Overall, this need to adjust to the educator role and manage a variety of challenges was often described by participants to be tiring or hard.
Theme 3: Educator and student relationship development
Despite the initial mixed feelings and challenges encountered, many participants reported that they enjoyed taking on the educator role, highlighting that the recency of their own student experience enabled them to relate to their students. They often described learning collaboratively with their students. One participant, when talking about learning work processes that she was unfamiliar with, explained “you just kind of do it together” [referring to her student] (P2). Participants also valued their student’s input with client care and appreciated “having a sounding board and an extra set of eyes in difficult scenarios to help with gathering evidence…” (P6). Within the educator-student relationship, educators also often sought feedback from their students on their performance as educators: “I’m more than happy for feedback for myself as well because that’s how we all learn” (P10).
Theme 4: Important support factors
Four important support factors, or subthemes were identified from the data (Fig. 1). These included tailored educator preparation, placement design, access to timely resources, and staff support. These factors were interconnected, with one factor often reliant on the presence of another.
Educator preparation
When preparing to be an educator, the desire to feel “comfortable” and “confident” within their caseload before taking on the educator role was expressed by multiple participants. One participant explained this further: “I was nervous about rotating to a new ward and having to familiarise myself while also familiarising my student as well” [to the caseload] (P8). To prepare themselves for the educator role, many participants appreciated the opportunity to observe other health professionals with their students or take another health professional’s student for a limited time.
The preparation meeting with a dedicated clinical education support staff member was highly valued by all participants. One participant believed, echoing the response of others, that this meeting was “a good opportunity to ask those questions that were burning in anticipation of having this [a] student” (P1). Discussing the use and location of placement resources, placement details and processes, and student feedback approaches during these meetings was greatly valued. Participants also found discussion on how to approach the educator role with other more experienced clinical educators aided their preparation. Furthermore, attending a clinical educator workshop was considered most useful by participants shortly before placement commencement, to facilitate information recall and utilisation. Views on whether workshop content met learning needs varied among participants.
Placement design
Sharing the educator role with a clinician more experienced in clinical education was found to be helpful by all participants who experienced this approach: “I think that’s a really nice way of stepping into that CE [clinical educator] role with sharing it with someone else” (P7). The experienced clinicians guided the participants to set clear student expectations, provide feedback, complete the student evaluation document, and supported the participants’ workload management. Sharing the educator role also assisted the participants in reflecting on and developing their own educator skills. Although sharing the role was considered unanimously helpful, one participant spoke of the “time-consuming” (P9) nature of effectively communicating with each other when sharing the role. Another participant considered the impact of a student being exposed to two educator approaches to clinical care: “we have different ways we do things” (P1).
Participants found consistent caseloads and having patients with similar presentations that students could work with helped to facilitate student learning. Highlighting this point, one participant voiced “I think because the clinical caseload is day in and day out quite similar you pick things up really quickly and you can run with it. And then you have that extra time to spend to educate and supervise and train someone else” (P1). Incorporating quality student placement learning activities that were not dependent on the educator’s presence enabled the participants to balance work duties. Examples participants shared included student project work, self-directed learning, peer sessions with other students, or spending time with other staff: “if there was a day … I needed to sit in the office and just get stuff done and get on top of things, not have to explain anything. We’d organise [student name] to go out …. with [colleagues name]” (P2). They also appreciated the time and space away from their students that these activities provided: “It was a nice balance for me to have breathing time on my own and doing my own thing” (P8).
Timely resources
Various resources assisted the participants in performing the educator role and facilitating student learning, including resources that helped to communicate their expectations to their students: “We used the student activity plan early on to set expectations about when we would expect [the student] to achieve certain things by” (P6). Weekly supervision templates that linked to the overall student evaluation document were also appreciated and supported student goal setting, with one participant admitting that “it’s really hard to keep track of everything, which obviously those supervision templates really helped” (P1). Additionally, “orientation checklists (P5)”, “tools to use for reflection” (P4), and a variety of treatment planning, feedback and project planning tools were also utilised. These resources came from a mixture of local, state-wide, or university sources. Frequently more experienced staff guided participants’ timely use of resources.
Staff support
Participants frequently reported needing support from staff more experienced in clinical education. This included dedicated clinical education staff, the clinician’s supervisor, peers, work team members, and university placement staff. This support assisted participants with educator skill development. Expectations for student learning, the provision of feedback, and the completion of the student evaluation document were common topics discussed. Participants appreciated receiving reassurance from experienced staff regarding their approach to facilitating student learning: “[meeting with an experienced staff member] was really valuable, just to validate that I’m on the right track or just [get] some tips.” (P5). They were also grateful for the emotional support the experienced staff provided. When referring to using their own supervision time during placement, one participant described it as “just a place to debrief, sometimes it’s needed” (P9). Participants valued support from their work team to enable them to balance their workload. Helpful strategies of students spending time with other health professionals, team members, or team members assisting with the participant’s workload were identified by participants. This enabled “protected time” (P8) for participants to support student learning and complete the student evaluation document. Most participants reported feeling sufficiently prepared and supported in taking on the educator role.
Theme 5: Development of educator, clinical, and professional skills and confidence
Over the placement, participants felt that their skills in tailoring their educational approach to their students’ needs improved. They spoke of their ability to adapt to their students’ learning styles and give their students the right level of responsibility to build their autonomy: “…I think that initial just right challenge, I feel like I’ve started to navigate better” (P7). There was a common theme of educators needing to learn how to “observe and not intervene [during client interactions]” (P6) to facilitate student skill development.
Furthermore, participants developed educator and professional skills in communication, time management, leadership, and provision of feedback. One participant, when asked whether there was anything that they felt they had improved in over the placement, responded by saying “I think everything, just planning, giving concise feedback, [and] explaining things in a more concise way” (P4). Overall, participants felt that through the placement experience, their confidence as educators had improved, resulting in them feeling “a lot more confident to be able to take on another student” (P9).
Participants also described how teaching consolidated their clinical knowledge and skills: ‘’it reaffirms your own knowledge base” (P1). It also prompted them to reflect on their learning and skills, as they wanted to do their best as an educator: “when you’re having to teach someone, you go, wow, maybe I don’t know that as much as I should, and I should go brush up on that” (P9). This self-reflection led them to seek supervision or support from more experienced staff: “there were definitely a few things that I just wanted to confirm… so I felt confident in my competence” (P6). Some participants also described how they extended themselves clinically to provide more learning experiences for their students: “my clinical skills definitely improved whilst [student name] was there because I’d sought out opportunities that before I wouldn’t have sought out.” (P2). Specifically, many participants identified that their clinical reasoning was enhanced through needing to explain and justify their intervention choices to their students: “I just thought through, reasoned through things better” (P6).
link







More Stories
UniHealth Hospitals Limited Announces the Commissioning of its Advanced Tertiary Care, Multi-Specialty Hospital in Navi Mumbai
Predictors of opportunistic infections among people living with HIV: a prospective cohort study from a tertiary care setting in India
The impact of DRG payment reform on inpatient costs for different surgery types: an empirical analysis based on Chinese tertiary hospitals