Study Population
We analysed data from 238 PWH hospitalised at the participating institutions during the specified timeframe. From those 30 PWH were hospitalised in the private health care center. The participants had a median age of 38 years (interquartile range [IQR]: 30–49), of whom 10% (24/238) were female. Among the participants, 54% (128/238) had an ADE during their initial hospitalisation. 12% (28/238) received their HIV diagnosis during their first hospitalisation, a proportion that increased to 39% (92/238) when considering both the first hospitalisation and the preceding six months. For those with over six months of HIV diagnosis, the median duration from HIV diagnosis to the first hospitalisation was 8.1 years (IQR: 3.6–14.6).
Among 90% (214/238) of PWH, a CD4 + cell count was available, measured at a median of 29 (IQR: 9–78) days before the first hospitalisation event. The participants had a median CD4 + cell count of 125 cells/mm3 (IQR: 44–341). Furthermore, 87% (207/238) of PWH had a viral load measurement from a median of 32 days (IQR: 3–84) before their first hospitalisation. Among those with available viral load data, 62% (129/207) had VS.
Of the participants, 18% (42/238) were hospitalised due to COVID-19, while 82% (196/238) were due to non-COVID-19 causes. All participants hospitalized in the private center were classified in the non-COVID-19 group. Among those with COVID-19 diagnosis, 95% (40/42) had a positive RT-PCR test for SARS-CoV-2, while 5% (2/42) were supported by characteristic pulmonary CT image and a clinical trajectory strongly suggestive of COVID-19 pneumonia. Since oxygen support was the main requirement for hospitalization according to the local guidelines at the time, all PWH hospitalized due to COVID-19 required oxygen support due to acute respiratory failure. However, specific data regarding oxygen saturation at hospital admission was not collected for all patients [25]. A comparative analysis of patient characteristics for each group is detailed in Table 1.
Patients in the non-COVID-19 group were younger and had a lower median CD4 + cell count during hospitalisation, a higher proportion of ADEs, and a lower proportion of VS upon admission than PWH in the COVID-19 group.
Hospitalisation events
We identified a total of 300 hospitalisation events. Predominantly, 83% (198/238) of PWH experienced a single hospitalisation event during 2020. Those with multiple events had a median count of 2 (IQR: 2–3). PWH hospitalised due to non-COVID-19 causes demonstrated a higher proportion of two or more hospitalisations (20% vs. 2%, p < 0.01). A length of stay of at least 14 days during the initial hospitalisation was observed in 49% (116/238) of PWH. Considering all events, the median hospitalisation time for PWH was 14 days (IQR: 7–25), totalling 4,467 patient-days.
The primary reasons for first hospitalisation were ADEs (54%, 128/238), exclusive COVID-19 (16%, 39/238), and other causes (30%, 71/238). Among the identified ADEs, the most prevalent were Kaposi Sarcoma (KS) (26%, 33/128), Pneumocystis jirovecii pneumonia (23%, 29/128), tuberculosis (19%, 24/128), histoplasmosis (15%, 19/128) and non-Hodgkin Lymphoma (15%, 19/128). Among the PWH hospitalised due to COVID-19, three also had ADEs. All three had histoplasmosis, one had tuberculosis, and one had KS. Other causes of hospitalisation were non-ADE infections (61%, 43/71), elective surgeries (13%, 9/71), systemic diseases (13%, 9/71), non-ADE cancer or chemotherapy administration (8%, 6/71), urgent surgeries (3%, 2/71), mental health disorders (1%, 1/71) and pregnancy-related conditions (1%, 1/71).
Outcomes
The most common clinical outcome was discharge due to improvement, constituting 75% (179/238) of cases. Overall mortality was 18% (43/238), with 12% (5/42) of PWH in the COVID-19 group and 19% (38/196) in the non-COVID-19 (p = 0.36). In the non-COVID-19 group, 66% (25/38) of deaths were attributed to ADEs, while 24% (9/38) were attributed to non-ADE infections or malignancies, and 10% (4/38) were due to other causes. In this group, 5 deaths were recorded among the participants hospitalised in the private center. Among the PWH with COVID-19, 43% (18/42) required invasive mechanical ventilation (IMV), of which 78% (14/18) were intubated. All deaths in the COVID-19 group were due to Acute Respiratory Failure Syndrome, with four of them occurring during IMV. Additionally, two further deaths were observed in the non-COVID-19 group, occurring at 61 and 107 days after the final hospitalisation event. The first death resulted from an ADE, while the second was attributed to other causes.
In a Cox model examining mortality, an adjusted Hazard Ratio (aHR) of 2.63 (95% CI: 1.14–6.08, p = 0.023) was associated with AIDS diagnosis. As an admission diagnosis, COVID-19 was not associated with death, yielding an aHR of 0.86 (95% CI: 0.28–2.62, p = 0.79) compared to other admission causes (Figs. 1 and 2). Additional factors associated with mortality among hospitalised PWH are outlined in Table 2.
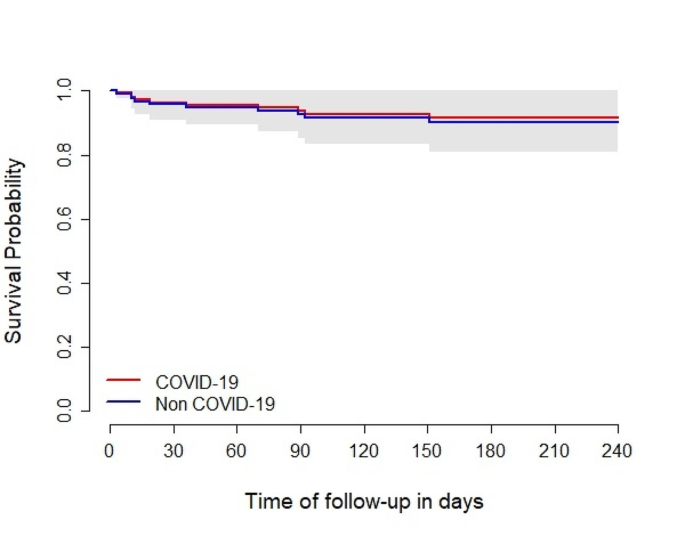
Adjusted survival probability since the first hospitalisation for COVID-19 vs. non-COVID-19. Note Adjusted survival from a Cox model for death, stratified by COVID group, including sex, age, COVID group, and the interaction between AIDS diagnosis and HIV diagnosis during hospitalisation. The curves are predicted survival curves using male sex, 40 years old, non-HIV diagnosis and non-AIDS status. The grey area depicts the 95% confidence interval
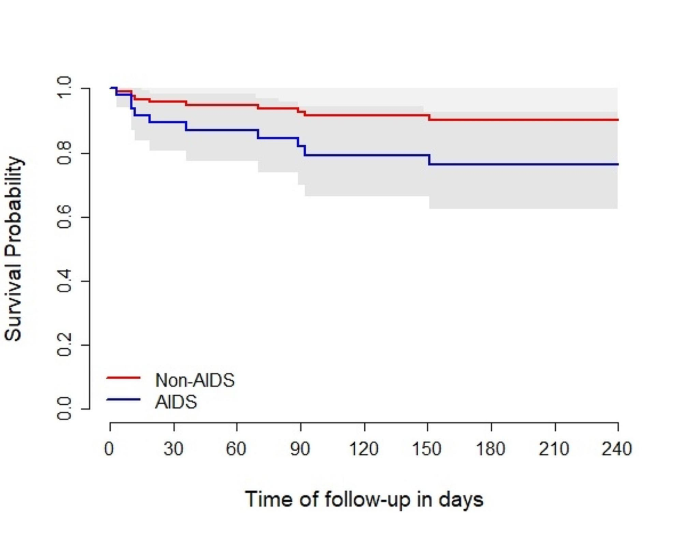
Adjusted survival probability since the first hospitalisation for AIDS vs. non-AIDS. Note Adjusted survival from a Cox model for death, stratified by COVID group, including sex, age, COVID group, and the interaction between AIDS diagnosis and HIV diagnosis during hospitalisation. The curves are predicted survival curves using male sex, 40 years old, non-HIV diagnosis during hospitalisation, and no-COVID status. The grey area depicts the 95% confidence interval.
General characteristics of hospitalisation events during 2019
To assess the impact of COVID-19 on hospitalisation and mortality among PWH, we compared the characteristics of PWH hospitalised in the same centres during 2019 and those in 2020. In 2019, we documented 812 events involving 556 PWH (Table 3). The median in-hospital duration was ten days (IQR: 6–16.2) accumulating to 11,131 patient-days. Among the PWH, 25% (140/556) experienced multiple hospitalisations, and 9% (51/556) died.
In comparison to 2019, we documented a decline of 57% in the total number of PWH hospitalised (238 vs. 556), along with a 60% reduction in total patient-days (4,467 vs. 11,131 days). Although the proportion of PWH experiencing more than one hospitalisation event was lower (17% vs. 25%, p = 0.01), the mortality among all PWH was significantly higher (18% vs. 9%, p < 0.01) in 2020 compared to 2019. Moreover, within the non-COVID-19 group, the mortality in 2020 was significantly higher than that observed in 2019 (19% vs. 9%, p < 0.01).
link







More Stories
UniHealth Hospitals Limited Announces the Commissioning of its Advanced Tertiary Care, Multi-Specialty Hospital in Navi Mumbai
Predictors of opportunistic infections among people living with HIV: a prospective cohort study from a tertiary care setting in India
The impact of DRG payment reform on inpatient costs for different surgery types: an empirical analysis based on Chinese tertiary hospitals